The Safest Vaccine In The World Is No Vaccine: TLFPGVG
Dangerous Vaccines Have Caused Kawasaki Pandemic For Children Globally And Now It Is UK’s Turn
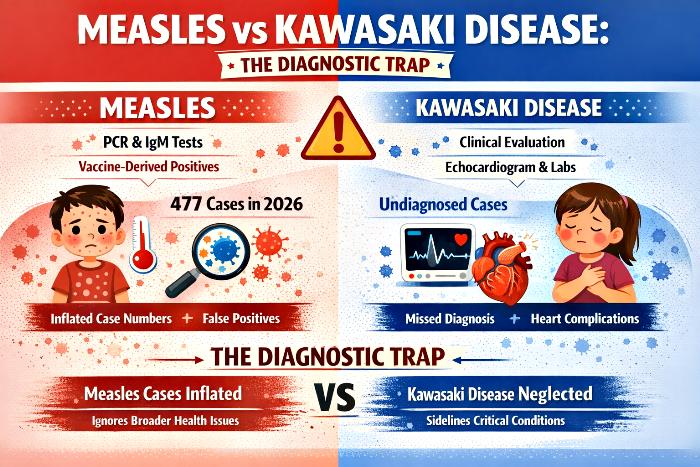
Measles Surveillance, Kawasaki Disease Neglect, And The Diagnostic Trap In The United Kingdom
Measles Surveillance: Strong But Skewed
The United Kingdom has reported 477 confirmed measles cases between January and April 2026, with two-thirds occurring in children under the age of ten. London and Birmingham have emerged as hotspots, though no deaths have been recorded this year. Historical data shows 2,911 cases in 2024 and 959 in 2025, highlighting the cyclical nature of outbreaks. While these numbers reflect a vigilant surveillance system, the methods used—primarily PCR and IgM assays—cannot distinguish between vaccine-derived signals and wild-type infection.
As a result, vaccinated children often test positive despite not being truly infected. Genotyping, which can differentiate strains, is essential but not routinely applied, leaving surveillance skewed and inflating measles statistics.
Kawasaki Disease: The Overlooked Threat
Kawasaki disease (KD) is a serious inflammatory syndrome in children that presents with fever, rash, and other symptoms similar to measles. Unlike measles, KD lacks pathogen markers and requires clinical evaluation, echocardiography, and blood markers for diagnosis. Without timely recognition, children face risks of coronary aneurysms and myocarditis. Alarmingly, vaccine safety monitoring systems have repeatedly recorded KD cases following multiple vaccines, including MMR, rotavirus, pneumococcal, and influenza. Yet these signals are often sidelined, leaving KD under-recognized in outbreak investigations and delaying life-saving treatment. This neglect reflects a dangerous imbalance in healthcare priorities.
The Diagnostic Trap
This imbalance creates a diagnostic trap. Measles counts are inflated by vaccine-derived positives, while KD cases are neglected. The over-reliance on pathogen-based assays means that syndromes without clear microbial markers, like KD, are underestimated. This distortion not only misrepresents the true burden of measles but also denies children timely access to intravenous immunoglobulin (IVIG) therapy, which is critical for preventing severe cardiac complications. Blind reliance on PCR and IgM tests, without clinical balance, risks turning surveillance into a misleading exercise that diverts attention from more urgent pediatric threats.
Historical Record Of Measles In The UK
| Year | Notifications (cases) | Deaths | Vaccine Milestone |
|---|---|---|---|
| 1900 | No official data available | No official data available | – |
| 1910 | No official data available | No official data available | – |
| 1920 | No official data available | No official data available | – |
| 1930 | No official data available | No official data available | – |
| 1940 | 409,521 | 8,402 | – |
| 1950 | 367,725 | 2,977 | – |
| 1960 | 159,364 | 1,709 | – |
| 1970 | 307,408 | 100 | Measles vaccine introduced (1968) |
| 1980 | 139,487 | 46 | Rubella vaccine introduced (1970) |
| 1990 | 13,302 | 2 | MMR introduced (1988) |
| 2000 | 1,241 (lab-confirmed) | 1 | – |
| 2010 | 1,742 (lab-confirmed) | 1 | – |
| 2020 | 79 (lab-confirmed) | 0 | – |
| 2026 | 477 (provisional, lab-confirmed) | 0 | – |
Sources: UK Health Security Agency (UKHSA), Office for National Statistics (ONS), GOV.UK historic measles notifications and deaths.
Analysis Long-Term Decline In Deaths
The official record shows a steady reduction in measles deaths from the mid‑20th century onward. In 1940, measles caused over 8,000 deaths in England & Wales. By 1950, this had fallen to under 3,000, and by 1960 to around 1,700. By 1970, deaths were recorded at 100, and by 1990 only 2. After 2000, deaths were essentially eliminated. This decline is clear in the official surveillance data, regardless of interpretation.
Analysis 2: Persistence Of Infections Despite Falling Deaths
Even as deaths declined, measles infections remained high for decades. Notifications in 1940 exceeded 400,000 cases, and even in 1970, over 300,000 cases were reported. By 1980, cases were still above 100,000. It was only in the 1990s and 2000s that confirmed cases dropped to the low thousands or hundreds. This shows that measles continued to circulate widely in the population long after deaths had fallen, suggesting that improvements in nutrition, sanitation, and healthcare access played a major role in reducing mortality even before vaccines were introduced.
Analysis 3: Historical Milestones
The UK introduced the measles vaccine in 1968, rubella vaccine in 1970, and the combined MMR vaccine in 1988. These milestones are part of the official immunisation programme history. Alongside these milestones, the official record shows deaths continuing to decline and eventually reaching zero, while confirmed cases also fell to very low levels by the 2000s. However, the data also shows that deaths had already dropped dramatically before vaccines were introduced, pointing to broader public health improvements as a critical factor.
Blind Reliance On Vaccines: A Misguided Focus
The historical record demonstrates that measles deaths were already in steep decline before vaccines were introduced. Improvements in living conditions, nutrition, and healthcare access reduced mortality to negligible levels by the 1960s. Blind reliance on vaccines risks misdirecting healthcare priorities, creating a false sense of security while other conditions—like Kawasaki disease—are sidelined. When surveillance systems focus narrowly on pathogen detection and vaccine coverage, they overlook broader determinants of child health and fail to recognize syndromes that require urgent clinical attention.
A Replicable Model Without Over-Reliance On Vaccines
The decline in measles deaths before vaccines shows that public health improvements—better nutrition, reduced overcrowding, improved sanitation, and stronger healthcare systems—were powerful tools in reducing mortality. This model can still be replicated today. By investing in holistic child health, strengthening clinical diagnostic capacity, and ensuring balanced surveillance, healthcare systems can protect children without falling into the trap of vaccine-only thinking. Vaccines can remain part of the toolkit, but they must not become the sole focus at the expense of broader pediatric care.
Conclusion: From Vigilance To Balance
The UK’s measles surveillance system demonstrates technical rigor, but its imbalance has dangerous consequences. By overlooking Kawasaki disease, children risk preventable cardiac complications. The historical record shows that measles deaths declined dramatically even before vaccines were introduced, reminding us that broader public health improvements are equally vital. Blind reliance on vaccines and pathogen-based assays misdirects healthcare, inflates measles statistics, and sidelines urgent conditions like KD.
The path forward is clear: surveillance must evolve from narrow vigilance to balanced care. Genotyping should be used to refine measles detection, KD must be systematically recognized, and public health must embrace holistic child health strategies. Only then can we ensure that vigilance does not become negligence, and that children receive the full spectrum of care they deserve.
