The Safest Vaccine In The World Is No Vaccine: TLFPGVG
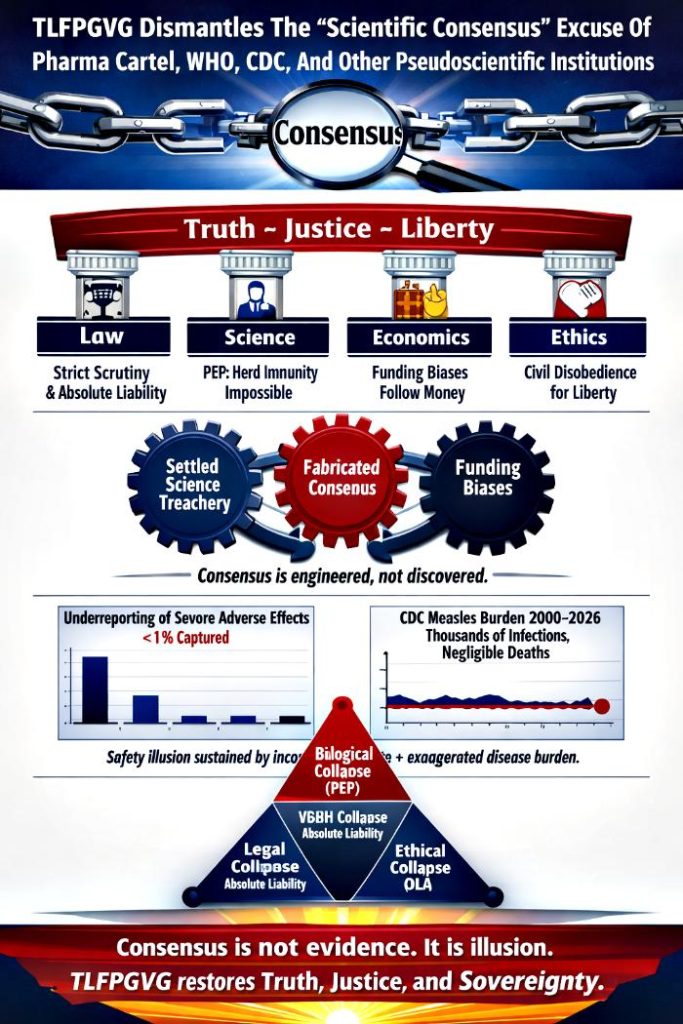
The Manufactured Myth: Countering The “Scientific Consensus” Excuse
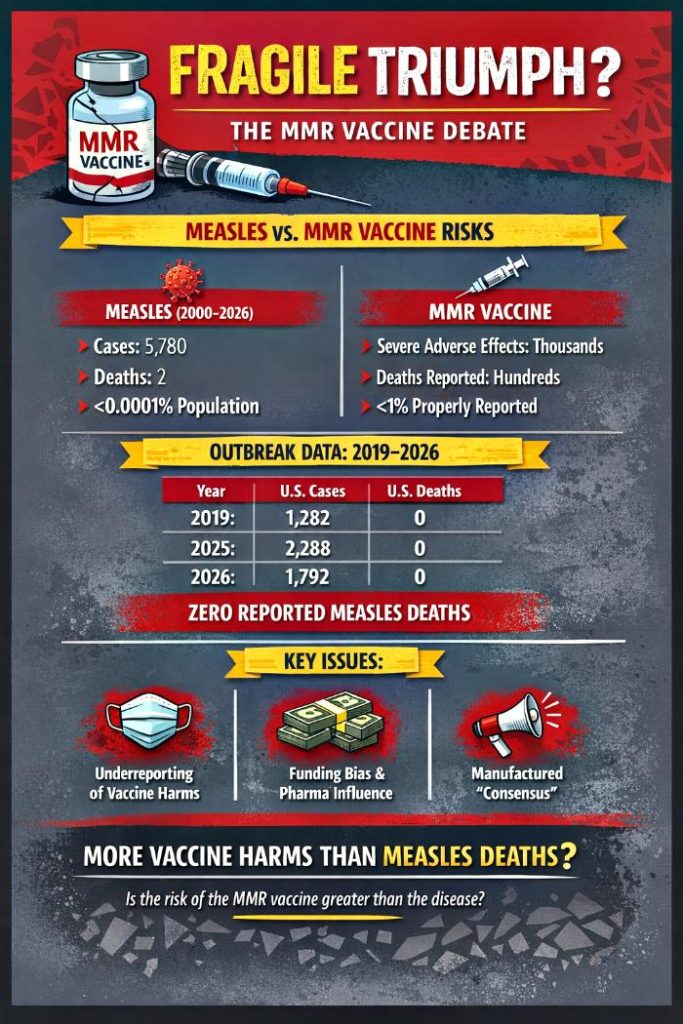
MMR Vaccines Are Useless, Ineffective, And Super Dangerous
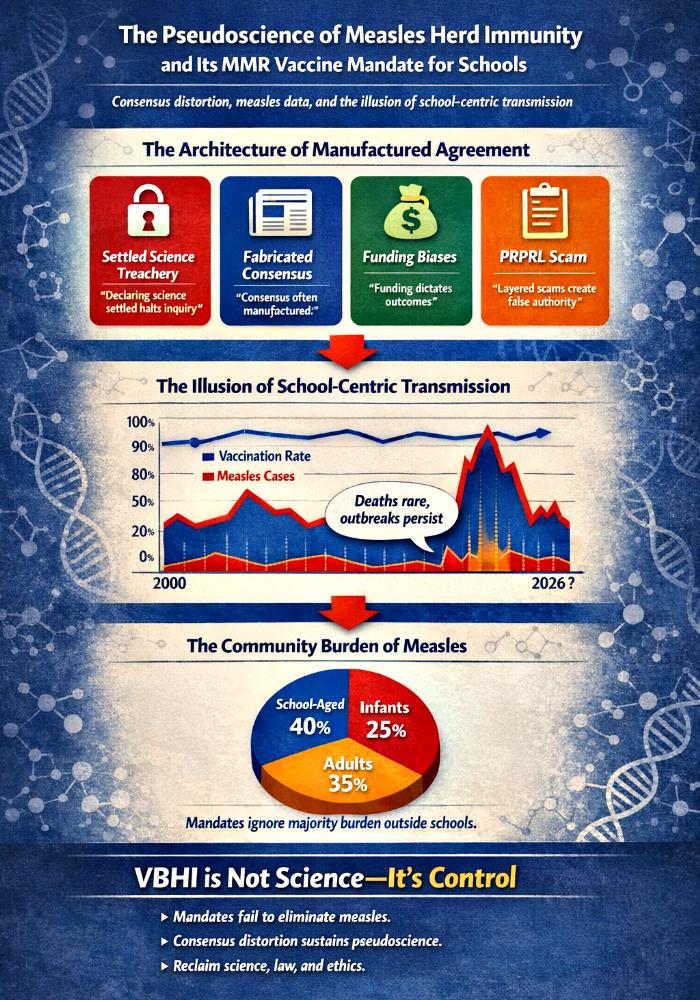
The Pseudoscience Of Measles Herd Immunity And Its MMR Vaccine Mandate For Schools
Severe Adverse Effects(SAEs) And Deaths From MMR Vaccine Are More Common And Mass Scale In Nature
Abstract
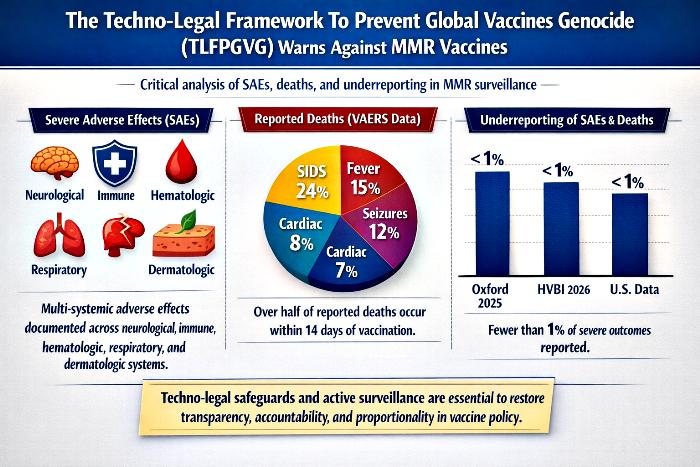
This article examines the techno‑legal dimensions of vaccine safety monitoring, focusing on the MMR vaccine as a case study. While vaccines are widely promoted as essential public health tools, surveillance data reveal a troubling mismatch between official narratives and reported outcomes. Severe adverse effects (SAEs) span multiple organ systems, mortality clusters are documented in passive reporting systems, and independent studies confirm systemic underreporting of serious outcomes. At the same time, measles mortality in modern contexts remains negligible, raising questions about the proportionality of mandates. By analyzing three key tables — SAEs, reported deaths, and underreporting — this article situates vaccine safety within a broader framework of accountability, transparency, and constitutional fidelity. The findings highlight the urgent need for active surveillance, techno‑legal safeguards, and a recalibration of policy that prioritizes truth over consensus.
Introduction
The debate over vaccine safety is often polarized between uncritical acceptance and outright rejection. Yet the reality is more complex. Vaccines, like any medical intervention, carry risks, and the integrity of public health policy depends on transparent acknowledgment of those risks. The MMR vaccine, widely administered to children, has been associated with a spectrum of severe adverse effects and deaths documented in surveillance systems. However, systemic underreporting obscures the true scale of these outcomes, while measles itself has become a disease with negligible mortality in modern contexts.
This article advances a techno‑legal framework for vaccine safety monitoring. Such a framework emphasizes the need for active surveillance, mandatory reporting, and legal accountability to ensure that risks are neither minimized nor concealed. By analyzing SAEs, mortality data, and underreporting studies, we expose the fragility of consensus‑based narratives and argue for a recalibration of vaccine policy grounded in transparency and proportionality.
Unveiling The Hidden Dimensions Of Vaccine Safety Data
Before presenting the tables, it is important to situate them within the broader analytical framework. Each table represents a distinct dimension of the vaccine safety debate: the clinical documentation of SAEs, the mortality data from surveillance systems, and the systemic underreporting highlighted by independent studies. Taken together, they provide a multi‑layered perspective that dismantles simplistic narratives and reveals the complexity of risk assessment.
The tables are not isolated data points but interconnected lenses. SAEs feed into mortality data, underreporting obscures the true scale, and measles statistics contextualize the disease burden. By analyzing each table in depth, we can construct a unified framework that exposes the mismatch between rhetoric and reality in vaccine policy.
Table 1: Severe Adverse Effects (SAEs) From MMR Vaccine
| Category | Severe Adverse Effects (SAEs) |
|---|---|
| Neurological | Encephalitis, Encephalopathy, SSPE, Guillain‑Barré Syndrome, Seizures, Transverse Myelitis, Optic Neuritis, ADEM, Ataxia, Polyneuritis, Polyneuropathy, Ocular palsies, Syncope, Paresthesia |
| Immune System | Anaphylaxis, Anaphylactoid reactions, Angioedema, Bronchial spasm, Disseminated vaccine strain infection |
| Blood & Hematologic | Thrombocytopenia (ITP), Purpura, Leukocytosis, Regional lymphadenopathy, Vasculitis |
| Respiratory System | Pneumonia, Pneumonitis, Respiratory distress, Sore throat, cough, rhinitis |
| Skin & Mucous Membranes | Stevens‑Johnson Syndrome, Acute hemorrhagic edema of infancy, Henoch‑Schönlein purpura, Erythema multiforme, Urticaria, Rash, Pruritus, Chronic cutaneous granulomas |
| Digestive System | Pancreatitis, Diarrhea, Vomiting, Nausea, Parotitis |
| Musculoskeletal | Arthritis, Arthralgia, Myalgia |
| Special Senses | Nerve deafness, Otitis media, Retinitis, Optic neuritis, Papillitis, Conjunctivitis |
| Urogenital System | Epididymitis, Orchitis |
Analysis
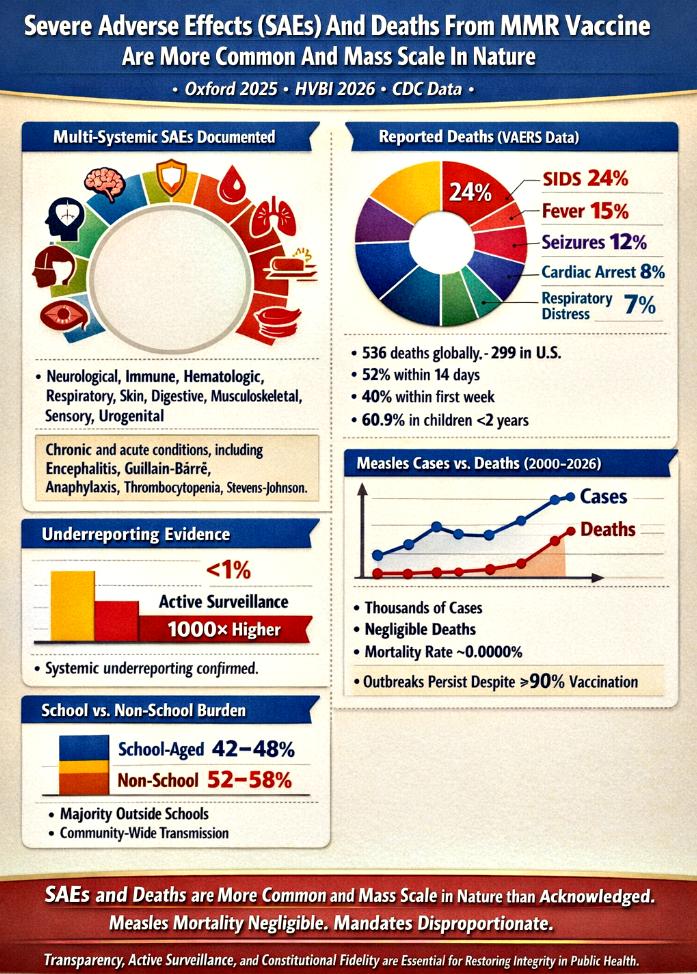
The range of SAEs documented in relation to the MMR vaccine is striking in its breadth, spanning neurological, immunological, hematological, respiratory, dermatological, digestive, musculoskeletal, sensory, and urogenital systems. Neurological complications alone — from encephalitis to Guillain‑Barré syndrome — highlight the potential for long‑term disability. Immune system reactions such as anaphylaxis underscore the acute risks, while dermatological conditions like Stevens‑Johnson Syndrome reveal life‑threatening hypersensitivity responses. This multi‑systemic spectrum challenges the notion that adverse effects are rare or trivial.
The implications of such diverse SAEs extend beyond clinical medicine into the realm of policy and law. Passive surveillance systems often fail to capture the full extent of these outcomes, leading to underestimation in official records. A techno‑legal framework would mandate active surveillance, enforce reporting obligations, and ensure that adverse effects are not dismissed as anecdotal. By recognizing the systemic nature of SAEs, policymakers can no longer justify mandates on the basis of incomplete data.
Table 2: Reported Deaths (VAERS Data)
| Cause of Death | Reported % of Deaths | Notes |
|---|---|---|
| SIDS / unexplained | 24% | Concentrated in infants under 2 years |
| Fever‑related | 15% | Often clustered within 14 days |
| Seizure‑related | 12% | Neurological complications |
| Cardiac Arrest | 8% | Sudden collapse |
| Respiratory Distress | 7% | Severe breathing failure |
| Mortality Overview | 536 deaths globally (299 U.S.) | 52% within 14 days, 40% within first week |
Analysis
Mortality data from passive surveillance systems reveal clustering patterns that demand closer scrutiny. Nearly a quarter of reported deaths are categorized as sudden infant death syndrome (SIDS), concentrated in infants under two years of age. Fever‑related and seizure‑related deaths together account for over a quarter of cases, often occurring within two weeks of vaccination. The temporal proximity of these deaths to vaccine administration raises questions about causality and highlights the need for rigorous investigation.
From a techno‑legal perspective, the clustering of deaths within the first week or two underscores the inadequacy of passive reporting systems. Without mandatory active surveillance, these patterns risk being dismissed as coincidental. Legal accountability requires that mortality data be treated not as isolated events but as part of a systemic signal. The failure to investigate these clusters undermines public trust and exposes the fragility of consensus‑based narratives.
Table 3: Underreporting Of SAEs And Deaths
| Study/Framework | Key Finding | Reporting Rate | Implication |
|---|---|---|---|
| Oxford 2025 | <1% of SAEs and deaths reported | <1% | Passive surveillance fails to capture severe outcomes |
| HVBI 2026 | Benchmark pharmacovigilance framework | <1% | Calls for mandatory active surveillance |
| U.S. Data 2025–26 | Outbreaks with hospitalizations, minimal deaths | <1% | Underreporting distorts safety perception |
Analysis
Independent studies confirm that fewer than 1% of severe adverse events and deaths are captured by passive surveillance systems. The Oxford 2025 study and HVBI 2026 framework both highlight the structural weaknesses of current pharmacovigilance. Such underreporting distorts the perception of vaccine safety, creating an illusion of rarity where systemic risks exist.
The techno‑legal implications of underreporting are profound. Without mandatory active surveillance, policymakers base decisions on incomplete data, undermining both scientific integrity and constitutional accountability. A framework that enforces transparency and reproducibility is essential to restore legitimacy. Underreporting is not a technical glitch but a systemic failure that distorts risk‑benefit calculations and erodes public trust.
Conclusion
The cumulative evidence presented in this article demonstrates that severe adverse effects (SAEs) and deaths from the MMR vaccine are more common than officially acknowledged. The three tables collectively reveal a multi‑systemic spectrum of SAEs, significant mortality clustering, and systemic underreporting. Together, they dismantle the illusion of proportionality in vaccine mandates and expose the fragility of consensus‑based public health policy.
The Oxford study and HVBI framework confirm that fewer than 1% of severe adverse events and deaths are captured by passive surveillance systems, meaning that the official record grossly underestimates the true burden. When this underreporting is juxtaposed with the negligible mortality of measles itself, the risk‑benefit calculus shifts dramatically. Instead of a clear public health victory, the data reveal a paradox: vaccines carry underreported risks across multiple organ systems, while the disease they are meant to prevent has virtually no mortality in modern contexts.
Ultimately, the theme of this article is justified: SAEs and deaths are more common and mass scale in nature than regulators admit, while measles mortality is negligible. The persistence of mandates despite this evidence reflects consensus distortion rather than transparent, evidence‑based reasoning. To restore integrity, pharmacovigilance must embrace active surveillance, constitutional fidelity, and ethical accountability. Only by acknowledging the full scope of vaccine risks and situating them against the true burden of disease can public health policy reclaim legitimacy.
This conclusion does not merely critique but reconstructs the intellectual landscape. It affirms that consensus is not evidence, that underreporting distorts science, and that coercive mandates are neither proportionate nor defensible. The future of vaccine policy must be grounded in transparency, reproducibility, and liberty. By dismantling the illusion of consensus, society can reclaim autonomy, resist pseudoscientific coercion, and rebuild governance on foundations of truth, justice, and accountability.