The Safest Vaccine In The World Is No Vaccine: TLFPGVG
Beyond The Banner Of Measles: Why Bangladesh’s Measles‑Like Symptoms (MLS) Crisis Is Not Measles
Abstract
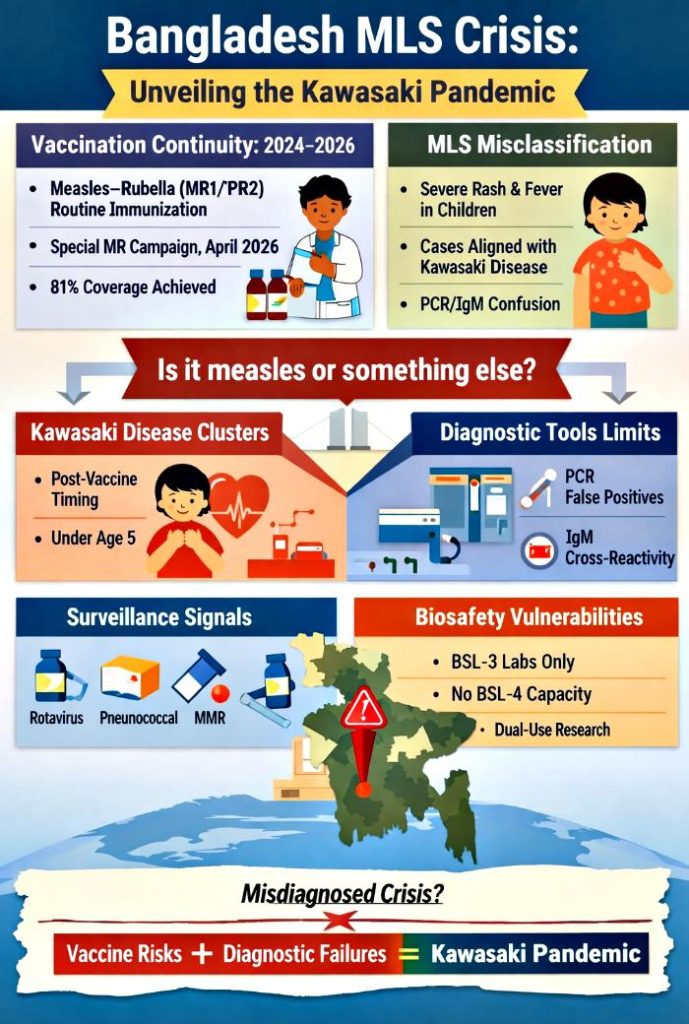
Bangladesh’s 2026 pediatric health crisis has been widely misrepresented as a measles resurgence caused by inadequate vaccination. This narrative, repeated across headlines and policy briefs, obscures the deeper reality. Evidence from the Expanded Programme on Immunization (EPI) shows that routine pediatric vaccination—including measles–rubella (MR)—continued uninterrupted from January 2024 through May 2026, even amid political upheaval. The special MR campaign launched in April 2026 achieved 81% coverage of target children, confirming that vaccine supply and delivery were not limiting factors.
Simultaneously, the outbreak was ambiguously framed as “measles” and “measles‑like symptoms (MLS).” Clinical and epidemiological data reveal that MLS cases clustered in children under five and aligned more closely with Kawasaki disease than measles. This diagnostic ambiguity, centered in Dhaka despite its concentration of sovereign BSL‑3 laboratories, highlights systemic fragility in outbreak classification.
This article integrates immunization data, diagnostic tools, vaccine surveillance signals, and biosafety infrastructure into a single framework. By reframing the outbreak as a convergence of vaccination continuity, diagnostic fragility, and biosecurity risk, we expose the deeper vulnerabilities of Bangladesh’s sovereign biosafety hub and underscore the urgent need for diagnostic clarity.
Introduction
Outbreak narratives often simplify complex realities into digestible headlines. In Bangladesh’s case, the 2026 pediatric crisis has been framed as a measles resurgence caused by inadequate vaccination. This framing is not only inaccurate but dangerous, as it obscures the real drivers of the crisis.
Routine immunization data show that Bangladesh’s EPI program continued to deliver vaccines—including MR—throughout 2024–2026, despite political upheaval and the July 2024 uprising. The special MR campaign launched in April 2026 achieved 81% coverage of target children, confirming that vaccine supply was robust. Yet the outbreak was simultaneously labeled “measles” and “measles‑like symptoms (MLS),” a vague construct that conflated two distinct clinical realities.
MLS cases diverged from measles in age distribution, prodrome, rash, and infectiousness, aligning instead with Kawasaki disease. This misclassification occurred in Dhaka, the epicenter of sovereign BSL‑3 laboratories, underscoring a paradox: advanced laboratory presence did not translate into diagnostic clarity.
The Immunization Backbone: Continuity Amid Crisis
Table of Resilience: Bangladesh’s National Pediatric Vaccination Schedule (Jan 2024 – May 2026)
| Vaccine | When given in EPI | Protects against | Approx. children per year* | Vaccine & supplier | Key partners (incl. NGOs) |
|---|---|---|---|---|---|
| BCG | At birth | Tuberculosis | ~3.0–3.3 million newborns | WHO‑PQ via UNICEF | Govt EPI, UNICEF, WHO, Gavi, NGOs |
| OPV | 6, 10, 14 weeks | Poliomyelitis | Same cohort; 3 doses | WHO‑PQ via UNICEF | Govt EPI, Global Polio partners, NGOs |
| IPV | 14 weeks | Poliomyelitis | Same cohort; 1 dose | UNICEF procurement | Govt EPI, WHO, NGOs |
| Pentavalent (DTP–HepB–Hib) | 6, 10, 14 weeks | Diphtheria, tetanus, pertussis, hepatitis B, Hib | Same cohort; 3 doses | WHO‑PQ via UNICEF | Govt EPI, Gavi, UNICEF, WHO, NGOs |
| PCV | 6, 10, 18 weeks | Pneumococcal disease | Same cohort; 3 doses | WHO‑PQ via UNICEF | Govt EPI, Gavi, UNICEF, WHO, NGOs |
| Rotavirus vaccine | 6, 10, 14 weeks | Rotavirus diarrhea | Same cohort; 2–3 doses | WHO‑PQ via UNICEF | Govt EPI, Gavi, UNICEF, WHO, NGOs |
| MR (Measles–Rubella) | MR1 at 9 months; MR2 at 15 months | Measles, rubella | Same cohort; 2 doses | WHO‑PQ via UNICEF | Govt EPI, Gavi, UNICEF, WHO, NGOs |
| Td | School‑age children; pregnant women | Tetanus, diphtheria | Millions annually | UNICEF procurement | Govt EPI, UNICEF, WHO, NGOs |
*Approximate birth cohort; exact dose counts not yet fully published.
Analysis
This schedule demonstrates the resilience of Bangladesh’s pediatric immunization program. Despite political unrest, the EPI system remained intact, covering millions of children annually. The inclusion of MR at 9 and 15 months directly counters the claim that measles vaccination was absent or inadequate.
The vaccination schedule also reveals how diagnostic ambiguity can emerge. Multiple vaccines associated with Kawasaki disease in global surveillance systems—including rotavirus, PCV, and DTaP—are administered within the first 18 weeks of life. This creates temporal windows in which KD may appear, particularly in a setting with limited diagnostic capacity. The overlap of MR campaigns with MLS cases magnifies the illusion of a measles outbreak.
The Convergence Of Vaccination, Diagnostics, And Biosafety
Master Consolidated Table – Bangladesh’s 2026 MLS Crisis: Vaccination, Diagnostics, Surveillance, and Biosafety
| Category | Aspect | Key Details (2024–2026) | Implications for MLS |
|---|---|---|---|
| Vaccination Continuity | Routine EPI schedule | MR1 at 9 months, MR2 at 15 months; uninterrupted delivery despite political unrest | Counters claim of vaccine shortage; continuity shows resilience |
| Special MR campaign | April–May 2026, >1.2M children targeted, 81% coverage achieved | Demonstrates robust supply and delivery; outbreak not due to vaccine failure | |
| Diagnostic Ambiguity | MLS construct | Fever, rash, conjunctivitis; overlaps with measles, KD, rubella, roseola, scarlet fever | Ambiguous category conflates distinct conditions; risks misclassification |
| Epidemiological pattern | Pediatric‑only cases; absence of adult infections | Aligns with KD’s age distribution; inconsistent with measles | |
| Diagnostic Tools | PCR | Detects viral fragments; contamination risk; false positives | Cannot confirm active measles infection; creates illusion of certainty |
| IgM | Detects early immune response; cross‑reactivity; timing variability | Prone to false positives/negatives; unreliable without clinical context | |
| Combined use | Suggestive evidence only | Cannot prove transmissible measles; misclassification risk | |
| Comparative Clinical Features | Measles vs KD | Measles: contagious, prodrome, descending rash, pneumonia/encephalitis; KD: non‑contagious, prolonged fever, polymorphous rash, coronary aneurysms | MLS features align more with KD; misdiagnosis delays appropriate treatment |
| Vaccine Surveillance Signals | Rotavirus | KD listed in FDA labels; trial imbalances | KD temporally associated with vaccination; complicates MLS attribution |
| Pneumococcal & DTaP combos | KD reports in VAERS and registries | Documented KD clusters within 0–42 days post‑vaccination | |
| Other vaccines | Hepatitis, Influenza, MMR, BCG | Temporal KD occurrences in surveillance systems | |
| MMR Paradox | KD onset | Median KD onset 8 days post‑MMR | Temporal overlap with measles campaigns; MLS may reflect KD misdiagnosis |
| Diagnostic certainty | 81% complete KD, 14% incomplete KD | Pediatric‑only MLS pattern consistent with KD, not measles | |
| Biosafety Infrastructure | National capacity | Multiple BSL‑3 labs; no BSL‑4 | Reliance on foreign labs for extreme‑risk pathogens; structural dependency |
| Oversight gaps | Use of BSL‑1/2 for high‑risk testing; ambiguous “BSL‑2+” designation | Raises containment and transparency concerns | |
| Partnerships | US CDC, USAID, Oxford, Global Fund; post‑2021 Chinese collaborations | Hybrid system; external reliance shapes outbreak narratives | |
| Regional Dynamics | Pakistan comparison | Allegations of dual‑use research with China; BSL‑4‑equivalent facilities | Regional asymmetry heightens Bangladesh’s vulnerability |
| Compliance | Bangladesh claims adherence to BWC | Needs stronger independent verification to maintain trust | |
| Narrative Bias | Official framing | Outbreak labeled “measles” despite atypical epidemiology | Simplified narrative obscures diagnostic fragility |
| Surveillance ecosystem | Optimized for measles detection (PCR/IgM kits) | Ambiguous cases default to measles, masking KD‑like syndromes |
Discussion
The dual evidence from the vaccination schedule and the consolidated framework demonstrates that Bangladesh’s pediatric crisis was not a vaccine failure but a diagnostic collapse. Vaccination continuity was strong, yet MLS cases aligned with Kawasaki disease rather than measles. PCR and IgM assays created an illusion of certainty, while surveillance signals and the MMR paradox reinforced the plausibility of misdiagnosis. At the same time, biosafety gaps and regional dynamics amplified structural vulnerabilities, leaving Bangladesh dependent on external partners for high‑risk pathogen analysis.
By integrating vaccination, diagnostics, surveillance, and biosafety into a single framework, the tables crystallize the central theme of this article: MLS in Bangladesh was misclassified due to systemic fragility and narrative bias. The convergence of these factors underscores the urgent need for sovereign diagnostic clarity, robust biosafety governance, and transparent investigation to restore public trust.
Conclusion
Bangladesh’s 2026 pediatric crisis cannot be understood as a simple measles resurgence caused by inadequate vaccination. Routine immunization continued uninterrupted, with MR vaccination achieving 81% coverage during the special campaign. The outbreak was misclassified, with MLS cases aligning more closely with Kawasaki disease than measles, and diagnostic ambiguity persisting despite Dhaka’s concentration of sovereign BSL‑3 laboratories.
Together, the evidence dismantles two misconceptions: that Bangladesh failed to vaccinate, and that the outbreak was measles. Instead, the crisis reflects systemic diagnostic fragility, narrative bias, and biosecurity vulnerability. Laboratory presence alone does not guarantee diagnostic clarity, nor does vaccine continuity prevent misclassification. To safeguard public health and national security, Bangladesh must strengthen diagnostic governance, decentralize laboratory reach, and confront structural biases in outbreak framing.
The lesson is clear: Bangladesh’s crisis was not a failure of vaccination, but a failure of narrative. By reframing the outbreak as a misclassified syndrome rather than a measles resurgence, we expose the deeper vulnerabilities of biosafety infrastructure and highlight the urgent need for sovereign diagnostic clarity.
